College of Pharmacy plays a crucial role in federally funded health care research in Nashville
Five faculty bring their expertise to patients at premier medical center.
Janel Shoun-Smith | 615-966-7078 |
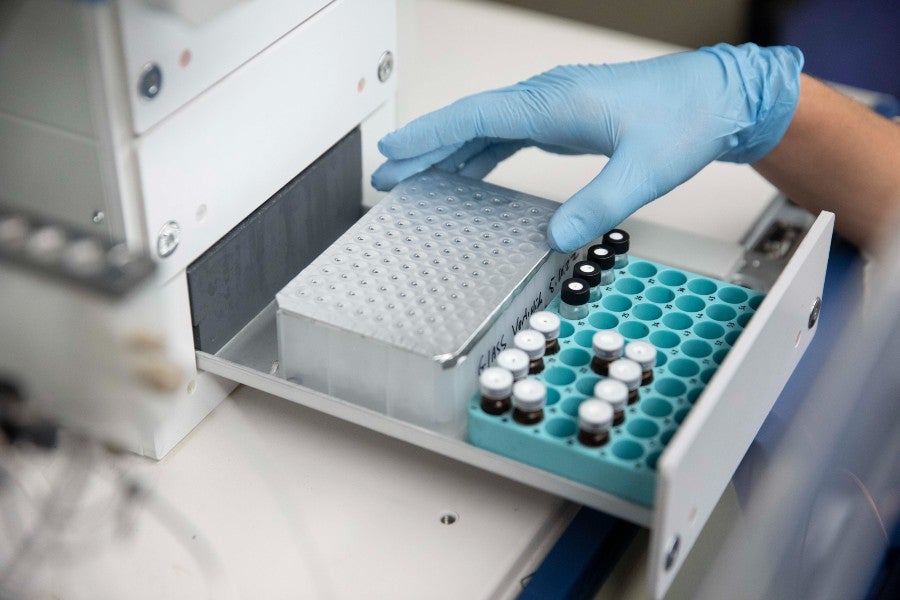
The scholars of Lipscomb University need no reminding to take full advantage of Lipscomb University’s prime location in Nashville, a thriving, growing city with a wealth of resources and opportunities for its residents and college students.
Lipscomb’s College of Pharmacy faculty with expertise in interprofessional education, drug development and clinical research are able to multiply the power of their scientific scholarship by teaming up with one of Nashville’s largest resources—Vanderbilt University, regularly ranked as one of the nation’s top universities, and Vanderbilt University Medical Center, one of the nation’s premier medical centers.
Through this long-time partnership, Lipscomb is maximizing opportunities to make a difference in the world on a national scale, and Lipscomb’s focus on involving students in hands-on research, means students can share a big role in that change-making as well.
In 2023-2024, the pharmacy college alone has five faculty working in tandem with Vanderbilt researchers on federally funded health care research projects. These faculty are implementing studies to explore the benefits of interprofessional patient care, medical devices, health care education enhancement and clinical trials for asthma medication and drugs used to help patients recover from acute heart failure.
Interested in partnering with Lipscomb College of Pharmacy on research? officeofresearch [at] lipscomb.edu (subject: Interested%20in%20Pharmacy%20Research) (Email the Office of Research and Grants.)

Scott Akers
Dr. Scott Akers
Executive Director of Pharmaceutical Sciences Research & Associate Dean of Research
TEAM Trial: Dose escalation clinical trial of high-dose oral montelukast to inform future RCT in children with acute asthma exacerbations
Funded by the National Institutes of Health’s National Heart, Lung, and Blood Institute; Vanderbilt’s Primary Investigator: Dr. Don Arnold
In July 2023, Akers began working on a clinical trial in pediatric patients who come to the emergency room suffering from acute asthma attacks. The study is testing whether the drug montelukast, currently used to prevent asthma attacks on a daily basis, can also be used in high doses to treat children already in the midst of an acute attack in the emergency room.
In the current phase of the trial, staff at the Monroe Carell Jr. Children’s Hospital at Vanderbilt are treating children with the drug and taking blood samples to send to Lipscomb, where Akers and his student research assistant, Dana Dishman, measure the drug levels in the blood to help determine how much the next dose should be in the next group of subjects. The trial is expected to run for two years.
This type of study is an example of how pharmacokinetics can be used to understand how a drug is absorbed, distributed, metabolized and eliminated by the body, an area of expertise that research faculty in Lipscomb’s Pharmaceutical Sciences Research Center has developed over the past 17 years.
“Pharmacokinetics impacts the dosing of every drug on the market,” said Akers. “You have to understand how to control the blood levels in the body to make the drug safe and effective. While it’s important to understand how a drug works, you need pharmaceutical scientists to help design dosage regimens in different patient populations to bring the drug to market.”
Email scott.akers [at] lipscomb.edu (subject: Interested%20in%20Partnering%20on%20Research) (Scott Akers) if you are interested in partnering on research.

Scott Akers, Executive Director of Pharmaceutical Sciences Research & Associate Dean of research, with a pharmacy student in the laboratory.

Zac Cox
Dr. Zac Cox
Professor of Pharmacy Practice & Adjunct Professor at Vanderbilt University School of Medicine
ESCALATE Trial: A Randomized Trial of Protocolized Diuretic Therapy Compared to Standard Care in Emergency Department Patients with Acute Heart Failure
Funded by National Institutes of Health; Vanderbilt’s project Director: Dr. Sean Collins
Pollypill Trial: Polypill Strategy for the Evidence-Based Management of Heart Failure with Reduced Ejection Fraction in an Underserved Patient Population
Funded by National Institutes of Health; Vanderbilt’s project Director: Dr. Deepak Gupta
Since coming to Lipscomb in 2009, Cox’s main focus of research has been exploring various drug therapies to reduce diuretic resistance (the build-up of fluid and sodium in the body) in hospitalized acute heart failure patients. At any one point in time, Cox is carrying out around 10 clinical trials with Vanderbilt patients as either the primary investigator or a consultant.
The two primary clinical trials he is carrying out during the 2023-2024 year build on his past research by investigating novel medical therapies, or those that haven't been previously reported in the scientific literature, to treat patients with heart failure.
The ESCALATE trial is a multicenter trial enrolling 450 patients hospitalized with heart failure to a strategy of protocolized diuretic therapy guided by spot urine sodium concentrations through completion of intravenous diuresis compared to usual care. Cox was instrumental in designing the study and serves as the site investigator at Vanderbilt.
The Pollypill trial is investigating if combining the four core medications to treat heart failure into one pill can improve patient outcomes.
Email zac.cox [at] lipscomb.edu (subject: Interested%20in%20Partnering%20on%20Research) (Zac Cox) if you are interested in partnering on research.

Lipscomb’s fourth-year student pharmacists have the opportunity to carry out their advanced pharmacy practice experiences (APPEs) at Vanderbilt, working directly under Cox.

Susan Hamblin
Dr. Susan Hamblin
Assistant Professor of Pharmacy Practice
The Partial REBOA Outcomes Multicenter ProspecTive (PROMPT)
Funded by Prytime Medical Devices, Inc. with original funding from the U.S. Department of Defense; Vanderbilt’s Co-Investigators: Dr. Stephen Gondek and Dr. Bradley Dennis
Hamblin is the lead study coordinator for the Vanderbilt site, in a multicenter study of the efficacy and safety of the pREBOA-PRO™ catheter. REBOA stands for “resuscitative endovascular occlusion of the aorta.” It is a device used to slow internal bleeding in patients who are exsanguinating.
This prospective, observational study is investigating the efficacy and safety of the pREBOA-PRO catheter (designed to allow for partial aortic occlusion) compared to a historical control group of patients who received the original REBOA catheter. This trial began enrolling Vanderbilt patients in August 2023.
Vanderbilt is the lead site, so Hamblin has leadership roles among various study sites, as well as coordinating research personnel, screening patients, collecting data, helping with data analysis, leading the monthly all-sites meeting for Prytime and ensuring compliance with all institutional regulations.
Email susan.hamblin [at] lipscomb.edu (subject: Interested%20in%20Partnering%20on%20Research) (Susan Hamblin) if you are interested in partnering on research.

Sarah Uroza
Dr. Sarah Uroza
Associate Professor of Pharmacy Practice
Vanderbilt University School of Nursing (VUSN) Nurse Education, Practice, Quality, and Retention (NEPQR) Simulation Education Training Program
Funded by Health Resources and Services Administration; Vanderbilt’s Project Director: Dr. Christian Ketel
VUSN faculty, the Vanderbilt School of Medicine and the Vanderbilt School of Divinity are collaborating with Lipscomb’s College of Pharmacy to create experiential learning opportunities to prepare nursing students to efficiently address health equity for rural and underserved populations.
In 2023, the group began working to develop a three-day simulation education training for faculty to prepare them to use simulation-based technology. Uroza plans to use Lipscomb’s pharmacy students within the simulation training.
Simulation scenarios will involve advanced patient assessments, diagnosis and recommended follow-up in the context of social drivers of health, the common realities faced by patients in a socially under-resourced and medically underserved health care setting.
The group is developing evaluation metrics to test competence in priority areas of behavioral/mental health including homelessness, maternal and child health and aging.
Email sarah.uroza [at] lipscomb.edu (subject: Interested%20in%20Partnering%20on%20Research) (Sarah Uroza) if you are interested in partnering on research.
This grant is supported by the Health Resources and Services Administration (HRSA) of the U.S. Department of Health and Human Services (HHS). The Nurse Education, Practice, Quality and Retention Simulation Education Training Program is supported by HRSA under grant number 1 T48HP52038-01-00 as part of an award totaling $500,000 with 0% financed with non-governmental sources.
The contents of this article are those of the author(s) and do not necessarily represent the official views of, nor an endorsement, by HRSA, HHS, or the U.S. Government. For more information, please visit HRSA.gov.

College of Pharmacy to create experiential learning opportunities to prepare nursing students to efficiently address health equity for rural and underserved populations.

Jessica Wallace
Dr. Jessica Wallace
Associate Professor of Pharmacy Practice
The Caring for OutPatiEnts after Acute Kidney Injury (COPE-AKI)
Funded by the National Institutes of Health’s National Institute of Diabetes and Digestive and Kidney Diseases; Vanderbilt’s Primary Investigator: Dr. Edward Siew
This randomized study is designed to evaluate if a multimodal process of care intervention, delivering different types of therapy together, may improve outcomes in patients following hospitalization for acute kidney injury (AKI). This multicenter includes not only Vanderbilt University, but also Yale and Johns Hopkins universities and the Cleveland Clinic among its eight sites.
The goal is to determine if multimodal care intervention, including care by a pharmacist, nurse navigator and nephrologist plus home blood pressure and weight monitoring devices, will result in more "hospital-free days” and better patient-reported outcomes over three months and lower rates of major adverse kidney events and rates of recurrent injury over six months.
As the study pharmacist on the Vanderbilt intervention care team, Wallace evaluates appropriate drug dosing based on kidney function, nephrotoxic burden and drug interactions. She also helps educate patients about kidney injury, medications to avoid and medication adherence and assists with medication access and barriers to care.
Email jessica.wallace [at] lipscomb.edu (subject: Interested%20in%20Partnering%20on%20Research) (Jessica Wallace )if you are interested in partnering on research.